History and exam
Key diagnostic factors
common
arthralgia
Arthralgias are common among patients with hepatitis C virus (HCV)-related cryoglobulinemia. In a study of 114 patients with mixed cryoglobulinemia due to HCV, 45% of patients reported rheumatologic symptoms. Typical rheumatoid arthritis was found in 10% of patients and seronegative arthritis in 17% of patients. Patients lacking rheumatologic symptoms had an average cryocrit level of <0.5% in 50% of cases.[28]
Rheumatoid factor activity is commonly observed in patients with rheumatoid arthritis and in patients with chronic HCV infection. Anticyclic citrullinated peptide antibodies can help to distinguish patients with HCV-related arthropathy from patients with rheumatoid arthritis.[29][30]
weakness
Weakness was described, along with purpura and arthralgia, as a cardinal feature in a case series of 9 patients with mixed cryoglobulinemia.[20]
vasculitis
Commonly presents as purpura and leukocytoclastic vasculitis. Half of these patients may have demonstrable immune deposits in vessel walls.[3] More extensive involvement results in peripheral neuropathy and renal involvement. In one case series of 40 patients followed for 21 years, medium vessel-wall vasculitis affecting the gastrointestinal tract, central nervous system, muscles, lungs, and adrenals was seen in the autopsies of 9 patients.[3]
lower-extremity vascular purpura
May be intermittent and vary from isolated petechiae to severe vasculitic lesions complicated by ulcers. In patients with chronic purpura, skin discoloration may also occur. Purpuric outbreaks can occur at the same time of day, perhaps related to cryocrit levels.[15][Figure caption and citation for the preceding image starts]: Lower extremity palpable purpuraFrom the personal collection of Dr GS Kaeley [Citation ends].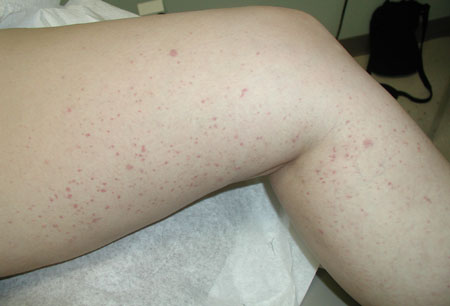
Other diagnostic factors
common
peripheral neuropathy
Commonly occurs with mixed cryoglobulinemia. The neuropathy predominantly affects the lower extremity. Sensory neuropathy is most frequently found, followed by motor neuropathy and mononeuritis multiplex.[32][33] Central nervous system involvement is rare but is associated with cognitive dysfunction and periventricular white matter changes on MRI.[34]
sicca symptoms
Half of patients with mixed cryoglobulinemia report sicca symptoms.[4] This may be related to concurrent hepatitis C virus (HCV) infection.
In a multicenter study, patients with HCV-related sicca syndrome more often had arthralgia, vasculitis, and neuropathy than primary Sjogren syndrome. This suggests an important role for cryoglobulinemia in the extraglandular features observed with sicca syndrome related to HCV infection. A higher prevalence of cryoglobulinemia, rheumatoid factor, and hypocomplementemia was observed. Seventy percent of HCV-sicca patients had a positive antinuclear antibody, but two-thirds of these had negative Sjogren syndrome antigens (SSA/SSB).[27]
hypertension
About one third of patients with mixed cryoglobulinemia (MC) may have renal involvement.[5][35] The presenting feature is usually proteinuria, hematuria, and arterial hypertension. Nephrotic and nephritic syndrome may occur in 25% of patients.[36]
Immunofluorescence testing may demonstrate intraglomerular subendothelial deposits of IgG, IgM, and complement components. Small-vessel vasculitis is rarely seen.[37][38] Early complement components (C1q, C4) are usually low. Development of uremia may occur in 20% of patients with MC after 10 years.[39]
uncommon
Raynaud phenomenon
May occur in about 25% of patients with type I cryoglobulinemia.[31]
lower extremity skin ulcers
The presence of lower extremity skin ulcers should raise the possibility of type I cryoglobulinemia.[1]
diplopia
Type I cryoglobulinemia may be complicated by life-threatening hyperviscosity syndrome. Signs and symptoms include bleeding, visual disturbances, diplopia, ataxia, headache, and confusion. Plasma or serum viscosity may be measured in patients presenting with these symptoms.[40]
ataxia
Type I cryoglobulinemia may be complicated by life-threatening hyperviscosity syndrome. Signs and symptoms include bleeding, visual disturbances, diplopia, ataxia, headache, and confusion. Plasma or serum viscosity may be measured in patients presenting with these symptoms.[40]
headache
Type I cryoglobulinemia may be complicated by life-threatening hyperviscosity syndrome. Signs and symptoms include bleeding, visual disturbances, diplopia, ataxia, headache, and confusion. Plasma or serum viscosity may be measured in patients presenting with these symptoms.[40]
confusion
Type I cryoglobulinemia may be complicated by life-threatening hyperviscosity syndrome. Signs and symptoms include bleeding, visual disturbances, diplopia, ataxia, headache, and confusion. Plasma or serum viscosity may be measured in patients presenting with these symptoms.[40]
retinal hemorrhage/retinal vein thrombosis
acrocyanosis
The presence of acrocyanosis should raise the possibility of type I cryoglobulinemia.[1]
Risk factors
strong
hepatitis C virus (HCV) infection
HCV infection may account for up to 90% of all cases of MC.[10][11][12] The highest rates of HCV infection in mixed cryoglobulinemia are found in the Mediterranean region.[13][14]
In patients with chronic HCV, cryoglobulinemia may be found in 20% to 56%, but less than one third of these are symptomatic.[2][4][15]
weak
other viral infections
autoimmune disorders
The most common autoimmune conditions associated with mixed cryoglobulinemia include Sjogren syndrome, systemic lupus erythematosus, scleroderma, undifferentiated connective tissue disease, and vasculitis.[9][17] However, some overlap with coexistent HCV infection, especially with Sjogren syndrome and polyarteritis nodosa, has been noted.
lymphoproliferative disorders
Type I cryoglobulinemia is most frequently associated with multiple myeloma, Waldenstrom macroglobulinemia, chronic lymphocytic leukemia, and B-cell non-Hodgkin lymphomas.[7]
The most common lymphoproliferative disorders associated with mixed cryoglobulinemia are Hodgkin and non-Hodgkin lymphomas. In one study, the presence of non-Hodgkin lymphoma was associated with HCV infection in 50% of patients with cryoglobulinemia.[9]
Use of this content is subject to our disclaimer