History and exam
Key diagnostic factors
common
rapid onset of signs and symptoms (acute septic CST)
The majority of patients have an acute presentation and present in a toxic state.
headache
fever
Occurs in almost all patients with septic CST.[41]
Is usually high.
periorbital edema
May be the earliest physical finding.
Together with chemosis and proptosis, these are the most consistent and visible features of septic CST.[15]
Caused by venous congestion within orbital veins.
Spread to the other eye within 24 to 48 hours of the initial unilateral periorbital edema is common and characteristic of septic CST.
chemosis and proptosis
Together with periorbital edema, these are the most consistent and visible features of septic CST.[13][15]
The sequential involvement of both eyes is indicative of acute septic CST.
Bilateral involvement is a late uncommon finding in the rare subacute septic CST.
[Figure caption and citation for the preceding image starts]: Patient with bilateral cavernous sinus thrombosis. Note the bilateral proptosis, which is more marked in the right eyeVidhate MR, et al. Bilateral cavernous sinus syndrome and bilateral cerebral infarcts: a rare combination after wasp sting. J Neurol Sci. 2011;301:104-106. Used with permission [Citation ends].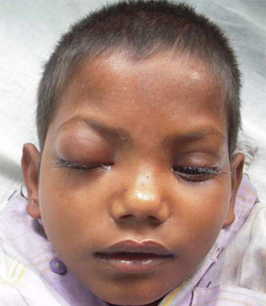 [Figure caption and citation for the preceding image starts]: Proptosis of the right eye in a patient with cavernous sinus thrombosis secondary to dental infectionJones RG, Arnold B. Sudden onset proptosis secondary to cavernous sinus thrombosis from underlying mandibular dental infection. BMJ Case Rep. 2009;2009. pii: bcr03.2009.1671. Used with permission [Citation ends].
[Figure caption and citation for the preceding image starts]: Proptosis of the right eye in a patient with cavernous sinus thrombosis secondary to dental infectionJones RG, Arnold B. Sudden onset proptosis secondary to cavernous sinus thrombosis from underlying mandibular dental infection. BMJ Case Rep. 2009;2009. pii: bcr03.2009.1671. Used with permission [Citation ends].
lateral gaze palsy
May precede full-blown ophthalmoplegia.
Unlike cranial nerves (CNs) III and IV, which are located in the lateral wall of the cavernous sinus and protected in a fibrous sheath, CN VI is situated medially and surrounded by blood, making it susceptible to inflammatory damage.
A unilateral isolated lateral gaze palsy is often an early sign in subacute septic CST.[15]
ophthalmoplegia
Develops as a result of cranial nerve involvement.
Often painful.
The sequential involvement of both eyes is indicative of acute septic CST.
Bilateral involvement is a late uncommon finding in the rare subacute septic CST.
profound sepsis (acute septic CST)
Including hypotension, tachycardia, and lethargy.
Seen in most cases of acute septic CST.
May help in differentiating septic CST from periorbital or orbital cellulitis.
Other diagnostic factors
common
ptosis and mydriasis
Owing to cranial nerve III palsy.
Mydriasis may be mid-size only (owing to sympathetic nervous system involvement in the cavernous sinus).
papilledema and/or retinal-vein dilatation
Seen in approximately 65% of cases.[15]
May help in differentiating septic CST from periorbital or orbital cellulitis.
decreased corneal reflex
Seen in less than 50% of cases.[1]
hypo- or hyperesthesia in the distribution of the ophthalmic and maxillary nerves
Signs can be subtle.
mental state changes (e.g., confusion, drowsiness, coma)
May occur secondary to central nervous system involvement and sepsis may develop rapidly.
clinically detectable primary infection site
An abnormal otolaryngologic exam, for instance, may include purulent nasal or posterior pharyngeal discharge, inflamed nasal mucosa, and tenderness over the sinuses.
meningismus (nuchal rigidity, photophobia, and headache)
Seen in as many as 40% of cases.[15]
May be due to concurrent bacterial meningitis or meningeal irritation.
Unlikely to be present in periorbital or orbital cellulitis.
positive Kernig or Brudzinski signs
May be due to concurrent bacterial meningitis or meningeal irritation.
Unlikely to be present in periorbital or orbital cellulitis.
uncommon
seizures
Should raise the suspicion of intracranial suppuration complicating septic CST.
loss of visual acuity
Reported in less than 50% of cases.[1]
Can be due to papilledema, corneal ulceration secondary to proptosis and loss of corneal reflex, occlusion of internal carotid, ophthalmic or central retinal artery, orbital congestion or embolic phenomena.
May help in differentiating septic CST from periorbital or orbital cellulitis.
Risk factors
strong
recent history of acute sinusitis
Most prevalent etiology in postantibiotic era.
The sphenoid and ethmoid sinuses are the most commonly involved.[7][8][9][10][13][15]
Infection from the sphenoid sinuses can spread through communicating veins, through osteomyelitis of the intervening diploic bone or mucosally, if there are bony defects.[39]
The infection from the ethmoid sinuses spreads indirectly through the ophthalmic veins, after breaching the lamina papyracea.[39]
history of facial infections
history of periorbital infection
Periorbital cellulitis may progress to CST.[41]
genetic prothrombotic condition
weak
history of otitis media, mastoiditis, or petrositis
The incidence of CST from middle-ear infections has declined owing to the introduction of antibiotics.
Infection spreads retrograde through the sigmoid sinus.
Organisms involved include Pseudomonas aeruginosa and coagulase-negative Staphylococcus.[42]
history of dental or oral infection
history of sepsis
Primary infection may occur at any other site (not just within the head) and includes bacterial meningitis.
immunosuppression
Mucormycosis (fungal infection of the sinuses, brain, or lungs, usually in people with immunosuppressive conditions) is a cause of septic CST.
May be either rhinocerebral or otocerebral.[16]
history of head and neck trauma
use of oral contraceptives
Cases of dural venous thrombosis have been reported to be associated with the intake of oral contraceptive pills.[48]
This is thought to be especially relevant to the third generation pills, containing gestodene or desogestrel.
pregnant or postpartum
Women who are pregnant or postpartum may be at increased risk.[4]
history of malignancy
Specifically, rhabdomyosarcoma, and nasopharyngeal carcinoma.[49]
history of recent head or neck surgery
vascular abnormalities
Including carotid-cavernous fistula.[33]
ulcerative colitis
One of several miscellaneous causes.
volume depletion
One of several miscellaneous causes.
heroin overdose
One of several miscellaneous causes.
Use of this content is subject to our disclaimer