History and exam
Key diagnostic factors
common
presence of risk factors
Key factors include increased humidity, poor hygiene, malnutrition and overcrowding, concomitant skin disease, chronic colonisation with Staphylococcus aureus (nasal, axillary, pharyngeal, perineal).[1]
vesicles/bullae
Seen in bullous impetigo. They are 2 cm in diameter or larger and initially clear, subsequently becoming turbid. Buccal mucosa may be involved.[Figure caption and citation for the preceding image starts]: Neonate with bullous impetigoFrom the collection of Michael Freeman; used with permission [Citation ends].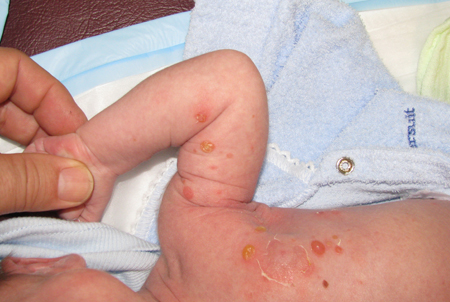 [Figure caption and citation for the preceding image starts]: Florid bullous impetigoFrom the collection of Michael Freeman; used with permission [Citation ends].
[Figure caption and citation for the preceding image starts]: Florid bullous impetigoFrom the collection of Michael Freeman; used with permission [Citation ends].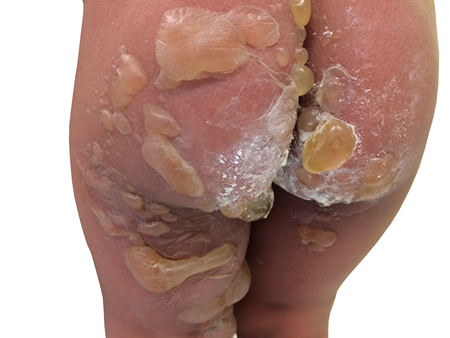
crusting
Impetigo usually presents a classic facial yellowish to golden crusting. The streptococcal form tends to have thicker and darker crusts.
In resolving impetigo, the crusts usually dry and separate, leaving an erythematous base. [Figure caption and citation for the preceding image starts]: Impetigo of arm presenting as an erosionFrom the collection of Michael Freeman; used with permission [Citation ends].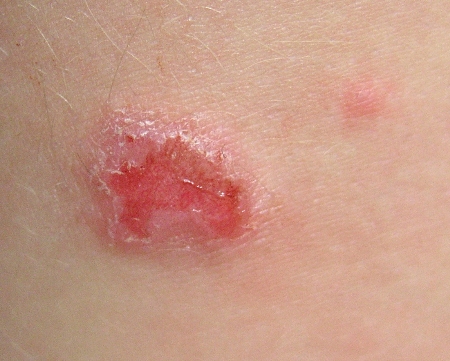
Other diagnostic factors
common
erythema
Patients often present with erosions that have a yellowish to golden crust on an erythematous base.
In resolving impetigo, the crusts usually dry and separate, leaving an erythematous base. [Figure caption and citation for the preceding image starts]: Facial impetigo, yellow crust no longer visibleFrom the collection of Michael Freeman; used with permission [Citation ends].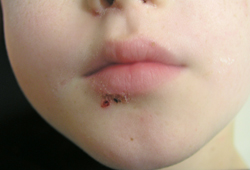 [Figure caption and citation for the preceding image starts]: Impetigo of arm presenting as an erosionFrom the collection of Michael Freeman; used with permission [Citation ends].
[Figure caption and citation for the preceding image starts]: Impetigo of arm presenting as an erosionFrom the collection of Michael Freeman; used with permission [Citation ends].
uncommon
pruritus
Occasionally pruritic.
pain
Rarely painful.
mucopurulent exudate
In non-healing cases, there is elevation of the crust by the underlying mucopurulent exudate of active disease.
lymphadenopathy
May occur with severe disease when large areas are affected.
fever
May occur with severe disease when large areas are affected.
Risk factors
strong
increased humidity
poor hygiene, malnutrition, and overcrowding
chronic colonisation with Staphylococcus aureus - nasal, axillary, pharyngeal, perineal
The anterior nares of up to 50% of children in a population may be colonised by S aureus.[9] The other noted sites of possible colonisation are less frequently involved. Recurrent episodes of impetigo can occur in people colonised by S aureus. Some of these individuals can be a point source for the spread of impetigo.
Use of this content is subject to our disclaimer