This blog provides further considerations regarding the neurological influence on distal musculotendinous junction injuries of the biceps femoris.
Introduction
Previous BJSM blogs (a and b) explored posterior thigh stretch combined with trunk flexion/rotation, with neural involvement, as a potential mechanism of injury for biceps femoris T-junction. This post further considers the neural components within our rehabilitation.
1) The nerves’ mobility:
91% of hamstring experts agree that “neural mobility could be considered” in treatment of hamstring injuries but that “the protection of the repaired or vulnerable tissue should be maintained” (1). Introducing torso and spine challenges during our hamstring exercises seems a very reasonable idea, with consideration of factors such as foraminal compromise, disc stress or lumbar instability to ensure we are protecting the nerves near their root. A skilled assessment of lumbopelvic mobility, stability and control might give us more confidence. More widely, such an assessment allows us to identify other lumbopelvic influences on hamstring injuries such as force closure, anterior pelvic tilt and pelvic asymmetry and address these as part of a comprehensive rehabilitation strategy (1).
2) Neuromuscular control and inhibition;
If the T-junction is a more complex neurological area, plus we’re seeing longer hamstring recovery times and/or higher re-injury rates, we might also consider the neurological process required to achieve an appropriate hamstring contraction.
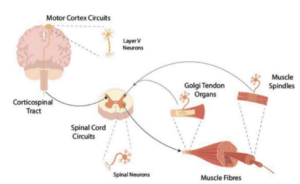
Figure 1: Considering the entire neurological process. Is it a software issue as well as a hardware issue? Picture taken from Haggie et al., 2023
Prolonged weakness (3) or eccentric-specific weakness (4, 5) may be signs of neurological inhibition. However, hamstring experts are yet to agree on whether inhibition plays a role in hamstring injuries (1). If it is considered, it might only be at the end of a rehabilitation process when we see chronic weakness despite adequate loading, or reinjury despite good tissue healing.

Figure 2: Neuromuscular inhibition is difficult to test for in a lab setting, let alone a clinical setting. But what clues might lead us to suspect it? Might it be an earlier consideration with T-junction injuries?
Concentric exercises do not appear to restore neuromuscular function, it is the eccentric component of strength exercises that appears to act as the stimulus for change (6). Lifting heavy is likely to increase neural drive which might also be a stimulus for neurological adaptation (7). However, our standard hamstring strength programmes routinely involve these elements anyway.
The below ideas should clearly not form the focus of hamstring rehab, but may be considered as creative adjuncts if we are suspecting neuromuscular inhibition. Might using them immediately before/during a strength session help an inhibited hamstring adapt to the subsequent training stimulus?
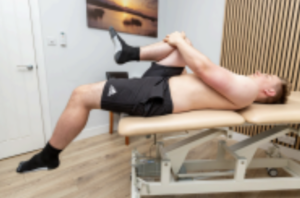
Figure 3: When one muscle has higher tone, its antagonist may be inhibited, termed reciprocal inhibition (8). With the biceps femoris, does its antagonists (hip flexors or knee extensors) have increased tone and can we reduce this?
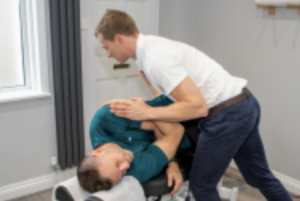
Figure 4: Spinal Manipulation may affect sensorimotor integration at the level of the brain. It may also result in strength changes into the lower limb lasting 30-60 minutes. Might manipulation have a positive downstream influence on the hamstring? (9,10,11)

Figure 5: An external pelvic compression belt has been shown to increase eccentric hamstring strength in terminal range between 5-10% on isokinetic testing (12,13) Longer-term, we might re-create some of the effect of this belt through progressive lumbopelvic strength/stability exercises that improve the force closure. (Picture taken from Arumugam et al., 2015).
Conclusion
- A general assessment of lumbopelvic mobility, stability and control might also be helpful as part of a complete hamstring management plan, particularly when looking to introduce additional torso movements into hamstring rehabilitation.
- Prolonged weakness or eccentric-specific weakness may be signs of neuromuscular inhibition. However, hamstring experts are yet to agree on its presence with hamstring injuries.
- Heavy loading and eccentric training might help address any neurological inhibition, but we could also consider more creative approaches in cases of chronic weakness or recurrent injury.
Author: Nick Metcalfe (LinkedIn) – Consultant Chiropractor with 16 years experience, including seven years consulting in the Premier League. Fellow of the Royal College of Chiropractors Sports Faculty, Member of BCA, BASEM and FMPA
References
- Paton BM, Read P, van Dyk N, Wilson MG, Pollock N, Court N, Giakoumis M, Head P, Kayani B, Kelly S, Kerkhoffs GMMJ, Moore J, Moriarty P, Murphy S, Plastow R, Stirling B, Tulloch L, Wood D, Haddad F. London International Consensus and Delphi study on hamstring injuries part 3: rehabilitation, running and return to sport. Br J Sports Med. 2023 Mar;57(5):278-291.
- Haggie L, Schmid L, Röhrle O, Besier T, McMorland A, Saini H. Linking cortex and contraction-Integrating models along the corticomuscular pathway. Front Physiol. 2023 May 10;14:1095260. doi: 10.3389/fphys.2023.1095260. PMID: 37234419; PMCID: PMC10206006.
- Fyfe JJ, Opar DA, Williams MD, Shield AJ. The role of neuromuscular inhibition in hamstring strain injury recurrence. J Electromyogr Kinesiol. 2013 Jun;23(3):523-30. doi: 10.1016/j.jelekin.2012.12.006. Epub 2013 Feb 9. PMID: 23402871.
- Opar DA, Williams MD, Shield AJ. Hamstring strain injuries: factors that lead to injury and re-injury. Sports Med. 2012 Mar 1;42(3):209-26. doi:10.2165/11594800-000000000-00000. PMID: 22239734.
- Sole G, Milosavljevic S, Nicholson HD, Sullivan SJ. Selective strength loss and decreased muscle activity in hamstring injury. J Orthop Sports Phys Ther. 2011 May;41(5):354-63. doi: 10.2519/jospt.2011.3268. Epub 2011 Feb 2. PMID: 21289455.
- Lepley LK, Lepley AS, Onate JA, Grooms DR. Eccentric Exercise to Enhance Neuromuscular Control. Sports Health. 2017 Jul/Aug;9(4):333-340. doi: 10.1177/1941738117710913. Epub 2017 Jun 1. PMID: 28571492; PMCID: PMC5496707.
- Tøien T, Haglo H, Nyberg SK, Rao SV, Stunes AK, Mosti MP, Wang E. Maximal strength training-induced increase in efferent neural drive is not reflected in relative protein expression of SERCA. Eur J Appl Physiol. 2021 Dec;121(12):3421-3430. doi: 10.1007/s00421-021-04807-0. Epub 2021 Sep 8. PMID: 34498135; PMCID: PMC8571128.
- Hamm K, Alexander CM. Challenging presumptions: is reciprocal inhibition truly reciprocal? A study of reciprocal inhibition between knee extensors and flexors in humans. Man Ther. 2010 Aug;15(4):388-93. doi: 10.1016/j.math.2010.03.004. Epub 2010 May 10. PMID: 20434390.
- Haavik H, Niazi IK, Jochumsen M, Sherwin D, Flavel S, Türker KS. Impact of Spinal Manipulation on Cortical Drive to Upper and Lower Limb Muscles. Brain Sci. 2016 Dec 23;7(1):2. doi: 10.3390/brainsci7010002. PMID: 28025542; PMCID: PMC5297291.
- Haavik Taylor H, Murphy B. The effects of spinal manipulation on central integration of dual somatosensory input observed after motor training: a crossover study. J Manipulative Physiol Ther. 2010 May;33(4):261-72. doi: 10.1016/j.jmpt.2010.03.004. PMID: 20534312.
- Christiansen TL, Niazi IK, Holt K, Nedergaard RW, Duehr J, Allen K, Marshall P, Türker KS, Hartvigsen J, Haavik H. The effects of a single session of spinal manipulation on strength and cortical drive in athletes. Eur J Appl Physiol. 2018 Apr;118(4):737-749. doi: 10.1007/s00421-018-3799-x. Epub 2018 Jan 11. PMID: 29327170; PMCID: PMC5843672.
- Arumugam A, Milosavljevic S, Woodley S, Sole G. Effects of external pelvic compression on form closure, force closure, and neuromotor control of the lumbopelvic spine–a systematic review. Man Ther. 2012 Aug;17(4):275-84. doi: 10.1016/j.math.2012.01.010. Epub 2012 Mar 2. PMID: 22386280.
- Arumugam A, Milosavljevic S, Woodley S, Sole G. Effects of external pelvic compression on isokinetic strength of the thigh muscles in sportsmen with and without hamstring injuries. J Sci Med Sport. 2015 May;18(3):283-8. doi: 10.1016/j.jsams.2014.05.009. Epub 2014 May 23. PMID: 24938927.